World Osteoporosis Day is observed on October 20. As a healthcare provider, preventing the onset and progression of this disease is on my mind year round. The purpose of this month’s blog post is to raise awareness about this multifactorial, preventable disease.
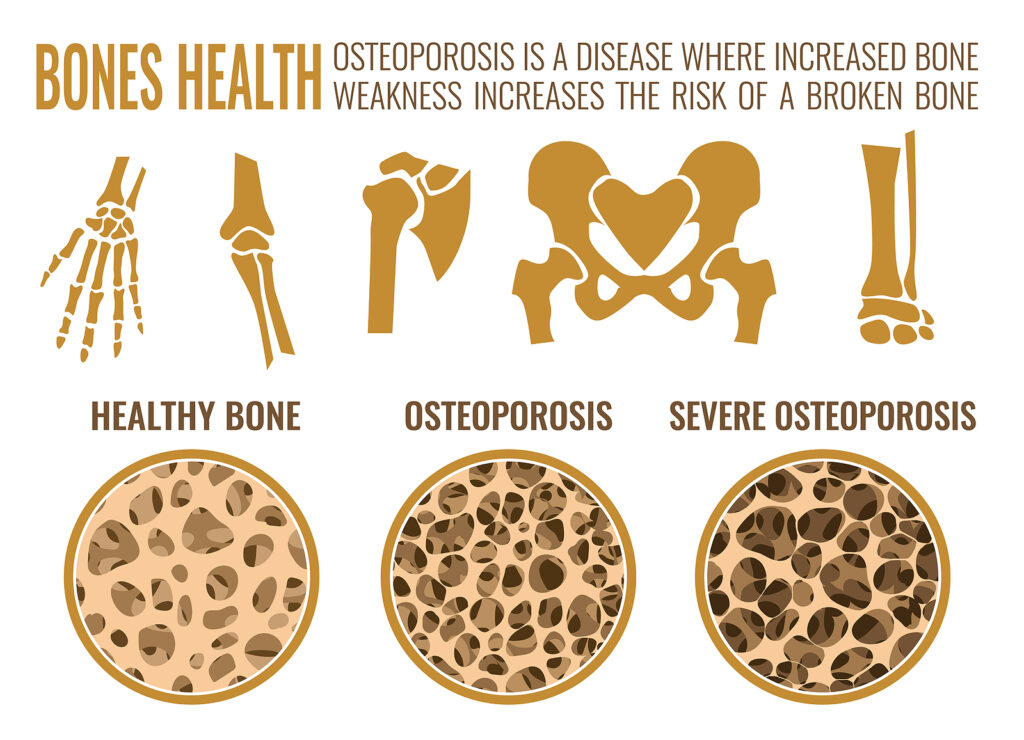
Osteoporosis is a skeletal disease characterized by loss of bone mass and density, which results in an increased risk of fractures. The disease is referred to as the “silent thief,” because it is often not evident until a person falls and breaks a bone from a minor fall. Common fracture sites include the lumbar vertebral spine (low back), hips and wrists. Osteoporosis accounts for 80% of fractures in people over 50. Osteoporosis-related fractures impair mobility, quality of life and independence. According to the National Institutes of Health, approximately 10 million people in the United States have osteoporosis and another 44 million are at risk for developing it.
Although osteoporosis is most prevalent in the elderly population, the disease begins several decades before it is detected. This is why it is important to promote bone health at all ages. Peak Bone Mass (PBM) is the greatest bone mass an individual attains in their lifetime. Typically, PBM is achieved between the ages of 18-25. Generally after PBM is achieved, most people will not lose much bone density for the next 20 years. However, decreases in bone density may start in the 30’s for people who have certain diseases, take certain medications or have other risk factors. Bones are living tissue and have cells that build bone (osteoblasts) and break bone down (osteoclasts). Therefore, like other cells in our body, cellular function of bone health is influenced by dietary, lifestyle, and environmental factors, as well as the health of the body’s other organ systems. Adequate levels of calcium, vitamin D, vitamin K2, magnesium and phosphorus are essential building blocks for bone strength. Many factors impair the absorption and excretion of these nutrients and contribute to decreased PMD.
Caffeine, nicotine and alcohol use are lifestyle factors that have been demonstrated to affect bone health. Excessive caffeine consumption interferes with absorption of nutrients that are needed to keep bones strong. Research demonstrates consumption of greater than 3 cups of coffee daily has a negative impact on bone health. Interestingly, black and green teas were not associated with having negative impacts on bone density. Nicotine and other chemicals found in cigarettes or vape pens negatively affect bone health by increasing bone turnover, decreasing production of cells that build bone and decreasing calcium absorption. Smoking these products also reduces blood supply to the bones and impairs nutrient delivery.
Certain disease states increase risk for osteoporosis. These pathologies result in decreased bone density from alteration of mineral and nutrient absorption, and increased bone turnover. Common contributing conditions include: celiac disease, irritable bowel disease such as Crohn’s disease and ulcerative colitis, rheumatoid arthritis, sarcoidosis, hyper/hypoparathyroidism, chronic kidney disease, and eating disorders (historical and active).
Frequent, prolonged or high doses of certain medications increases risk for osteoporosis by interfering with nutrients absorption or increasing bone loss. These medications include:
- Antacid medications known as proton pump inhibitors (Prilosec/omeprazole or Protonix/pantaprozole).
- Corticosteroids such as prednisone or dexamethasone.
- Depo-Provera contraceptive injection with more than 2 years of use.
- Methotrexate at higher doses for autoimmune disease management or in cancer treatment.
Adequate levels of sex hormones play an important role in maintaining bone density. During the first year of menopause, if not on hormone therapy, a woman’s estrogen levels decline by 80%. Estrogen loss causes increased bone turnover, decreased muscle mass and strength which contributes to balance issues and increased risk of falls. Male testosterone levels start to decline around 35-40 years of age. For most men, this decline is gradual at a rate of 1-3% per year. Decreased testosterone also contributes to bone loss and decreased muscle mass and strength.
Environmental exposures to heavy metals contribute to altered bone mineral density. Arsenic exposure alters osteoblast and osteoclast activity. Lead accumulates in bones making them weaker. Aluminum alters calcium and phosphorus metabolism and blocks calcium uptake into bones. Cadmium increases osteoclast activity, is especially toxic to kidneys, and causes mineral imbalances.
Weight bearing activity is important to build bone and maintain strong bones. Activities such as walking, jogging, hiking, dancing, gardening, pickleball and tennis are included in this category. Wearing a weighted-vest or a well-fitted backpack (one with sternum and lumbar straps) with an extra 5-10 pounds of weight while walking or hiking may enhance the bone building effects of these activities. Strength training at least 2 times per week is also beneficial to rebuild bone. Exercises to help maintain balance such as tai chi, pilates and yoga are also important for fall prevention. Certain yoga poses can be contraindicated in advanced osteoporosis.
The United States Preventative Task Force recommends screening for osteoporosis for all women beginning at age 65 or in younger postmenopausal women if they have risk factors.
Routine screening for men is not recommended, despite 1 in 5 men over age 50 sustaining an osteoporosis-related fracture. As a naturopathic doctor, I strongly believe in treating individuals not guidelines. It is often important to screen women and men who are younger than 65 based upon personal risk factors. Prevention and early detection are more effective than late treatment. Knowledge of individual risk factors help to prevent progression and reverse this disease.

